Osteochondrosis does not cause pain, but, at the same time, pain with osteochondrosis is possible. A strange, at first glance, situation. But, after you read this article, you will become a real expert not only on this issue, but also on: What is osteochondrosis? What are the reasons? What are the symptoms and signs? How to diagnose osteochondrosis? What effective treatment is there? What is included in the prevention of this disease? And also on many other issues.
What is osteochondrosis?
To understand what osteochondrosis is, you need to dive a little into history. The term was introduced in 1928 by Christian Georg Schmorl. But the curious thing is that Schmorl was a pathologist and, as you understand, he had no one to ask: "Where does it hurt? "(sorry for the dark humor). During his studies of pathological material, Schmorl discovered previously unknown changes at the junction of bone and cartilage, in particular in the area of the spinal discs. After these changes were described, all that remained was to come up with a name for them. To do this, he took the Latin word "bone" / os and the Greek word "cartilage" / chondros and, combining them, received the term osteochondrosis.
What is osteochondrosis, what exactly did Schmorl call this word? It turns out that this is not pain at all and, in general, not a sensation. With the word osteochondrosis, Schmorl designated the following three changes:
- decreased intervertebral disc height;
- subchondral sclerosis;
- marginal bone growths.
Translated into ordinary language, this means that the height of the disc has decreased, and the surface of the vertebra adjacent to the disc has become denser and grown in the form of a rim. This is what osteochondrosis is in its original meaning, which Christian Georg Schmorl put into it.
Disease osteochondrosis
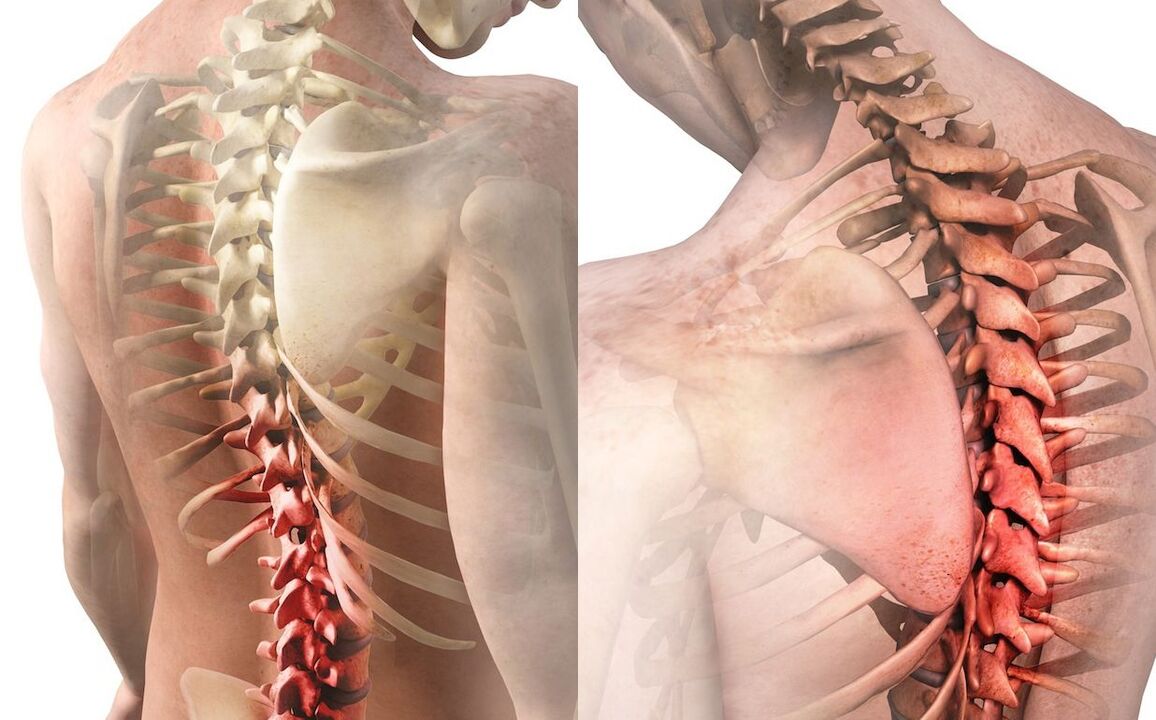
Let's once again pay attention to the fact that Schmorl did not describe the disease osteochondrosis, but only tissue changes, and these are different things. The concept of "disease" is much broader; it includes complaints, symptoms, laboratory and radiological changes, methods of treatment and prevention.
But Schmorl did not write about anything like that and, in general, did not consider osteochondrosis a disease. But why then is it customary to say that osteochondrosis is a disease, to be interested in the causes of its occurrence, its signs, symptoms and treatment of osteochondrosis?
But the fact is that Schmorl had followers. So they decided to find out how osteochondrosis manifests itself and what symptoms bother a person? As a result, it was found that osteochondrosis itself does not directly cause pain, as well as other sensations. This was explained by the fact that there are no pain receptors in the vertebrae and discs. And since there are no receptors, there can be no pain. This is easy to understand using the example of hair and nails - there are also no receptors or pain when they are cut.
The second important discovery was that osteochondrosis is part of a general degenerative process that covers all our organs and tissues. Dystrophy is a violation of tissue nutrition at the cellular level; it lasts throughout life and gradually ages our body. That is, osteochondrosis is essentially part of the aging process. But, as you know, details matter. And the details are that not all degenerative processes are as painless as osteochondrosis. In particular, dystrophic pathology of the muscles surrounding the spine is almost always associated with pain. After all, muscles, unlike vertebrae and discs, have pain receptors. A typical example is myofascial syndrome. It usually occurs in parallel with osteochondrosis and is painful. Now, remember, at the beginning of the article we said that osteochondrosis itself does not cause pain, but pain is possible? So, it is precisely these cases, when painful pathology is added to painless osteochondrosis - the same myofascial syndrome - that perfectly explain the meaning of what has been said.
You may ask, where is the answer to the question, why is it customary to say that osteochondrosis is a disease? Well, actually, we have already approached it. The fact is that, although osteochondrosis itself is not, in fact, a disease, but being the starting point in the study of degenerative processes, the word "osteochondrosis" has taken root in our language so much that, over time, it has become a slang generalizing name for all diseases of the spine.
Causes of osteochondrosis
The reasons can be divided into external and internal.
Internal (endogenous) causes include, first of all, the degenerative process that we discussed above. This also includes genetic predisposition, as well as hormonal, mineral, vitamin, protein and other metabolic disorders, as a result of which bone and cartilage tissue do not receive the necessary nutrition. All these are so-called biological factors, which, of course, can be influenced, but doing so is quite difficult and expensive. In spite of this, there are simple and cheap ways that allow you to achieve no less convincing results by eliminating only external causes.
External (exogenous) reasons are considered to be a sedentary lifestyle, poor training of the spinal corset muscles, microtraumas of the back and spine, insufficient physical activity, the habit of slouching, "sedentary" work, constant stressful situations, lack of preventive visits to a chiropractor and much more.
As you can see, external reasons are largely due to either our wrong actions, for example, low physical activity, or our inaction and neglect of our health, for example, ignoring prevention.
Agree, external causes are much easier to eliminate than internal ones. Of course, there are patients who cannot do without drug treatment for internal causes, but there are only a few of them. In most cases, it is enough to get rid of the external causes of osteochondrosis in order to get convincing results at lower costs. This will require a little self-discipline, basic physical activity and periodic visits to a chiropractor.
Symptoms and signs of osteochondrosis
Symptoms and signs are usually divided into those that develop within the spine itself and those that are extravertebral in nature.
What do you think are the symptoms of osteochondrosis that cause more problems? In fact, a lot here depends not only on the symptoms themselves, but also on other factors: age, weight, the presence of concomitant diseases in the patient, etc.
But, let's return to the symptoms of vertebral osteochondrosis: as we said, they are vertebral, they are also called vertebral and extravertebral - extravertebral. Extravertebral symptoms, in turn, are also divided into two groups – reflex and radicular symptoms of osteochondrosis.
For simplicity, this classification of back symptoms is best represented as follows:
- Vertebrates/vertebral
- Extravertebral/extravertebral: radicular symptoms and reflex symptoms
Spinal symptoms of osteochondrosis include curvature of the spine (not to be confused with scoliosis), local pain, muscle tension and impaired mobility.
Radicular symptoms occur due to effects on the nerves exiting the spine. This is manifested by decreased reflexes, muscle weakness, impaired sensitivity and radicular pain.
And here it is necessary to explain that all our vertebrae, discs and "roots" have a certain designation. Therefore, we can talk about radicular symptoms only when all these symptoms and signs clearly indicate a specific "root", and not when any pain "from the bulldozer" is called radicular.
Very rare, but dangerous signs and symptoms of osteochondrosis are paresis, paralysis and disruption of the pelvic organs. They indicate the development of a spinal stroke. This is a serious complication of osteochondrosis, in which the radicular arteries are affected.
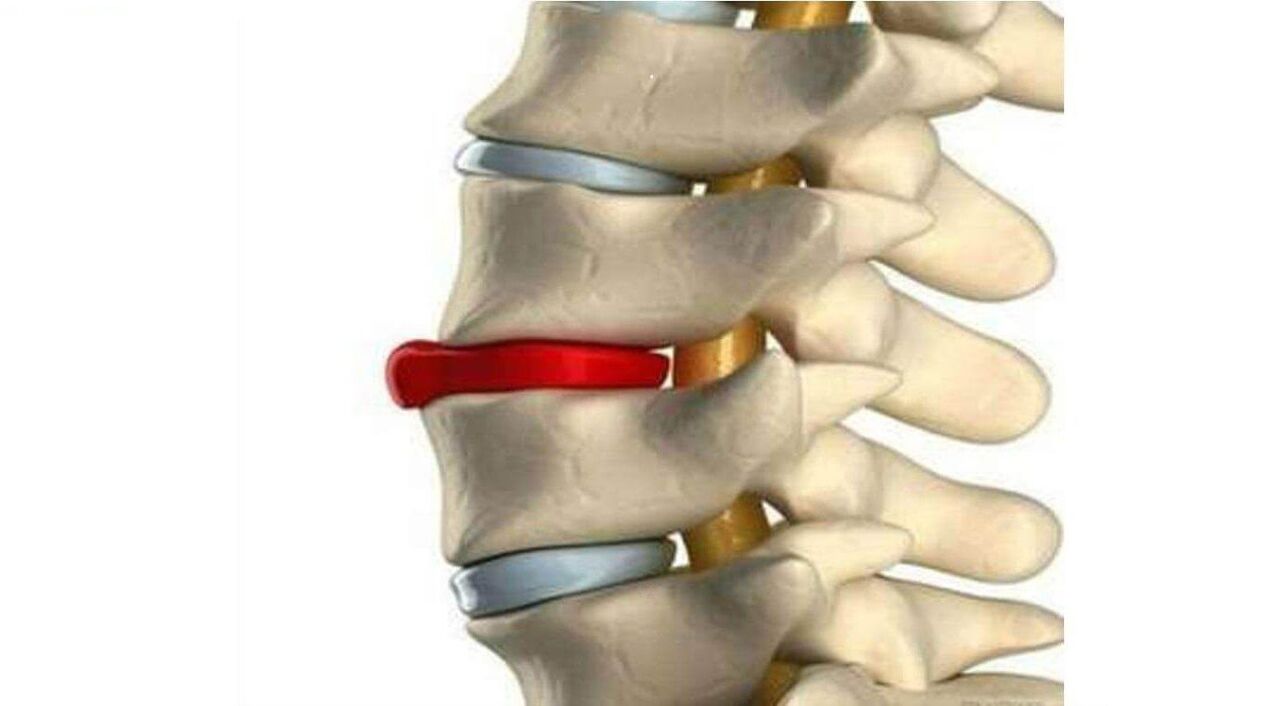
Reflex symptoms primarily depend on which part of the spine is affected. According to statistics, the cervical spine is most often affected.
The essence of cervical osteochondrosis is a large number of reflex symptoms. Pain in the neck, back of the head and collar area. Crunching of the vertebrae, muscle tension and difficulty moving. Headache. Dizziness. Intracranial pressure. Morning stiffness. Numbness, pins and needles, goosebumps and weakness in the arms. Pain in the shoulders and under the shoulder blade. Burning between the shoulder blades and in the area of the heart (reminiscent of angina). Numbness of the hands or fingers. "Lump" in the area of the seventh cervical vertebra. Temporary darkening or "floaters" in the eyes. Noise or ringing in the ears. Nausea, even vomiting. Pressure surges. Pre-fainting state. A lump in the throat with osteochondrosis, weakening of the voice, hoarseness, a feeling of lack of air, problems with swallowing and a sore throat with osteochondrosis - all these are quite common reflex symptoms. There may also be sleep disturbances, frequent insomnia, and feeling tired in the morning. General weakness. Irritability. Fast fatiguability.
As you can see, the symptoms and signs of the disease with osteochondrosis are very diverse. This is especially true for reflex symptoms.
Diagnosis of osteochondrosis
Diagnosis is the key to proper treatment. Modern hardware diagnostic methods make it possible to accurately confirm this diagnosis. As you know, MRI and CT are considered the most accurate examinations. But, as before, the main factor in making a diagnosis remains clinical diagnosis. This is when an experienced doctor compares data from at least three sources: the patient’s complaints, MRI results and the symptoms that were identified during the examination.
This approach to diagnostics allows you to establish an accurate diagnosis and develop an individual program of effective treatment.
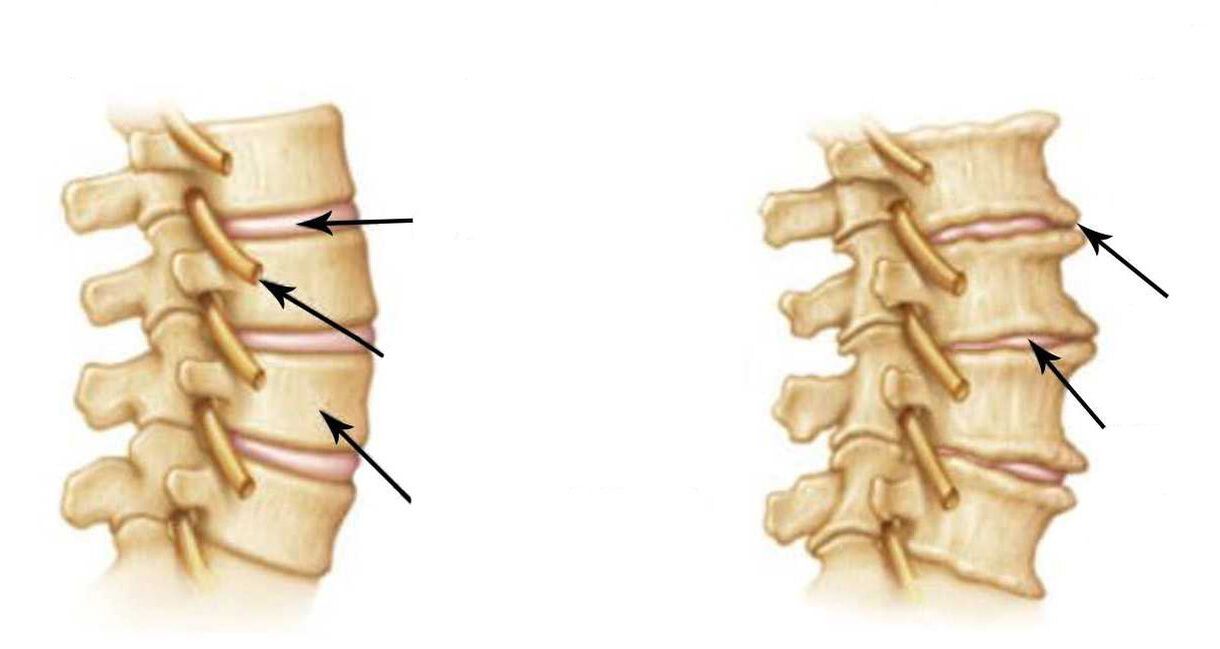
Effective treatment of osteochondrosis
Effective treatment of osteochondrosis is possible only with strict adherence to a scientific approach. This means that correct prioritization is necessary, first of all, in choosing the main and auxiliary types of treatment for vertebral osteochondrosis.
What do you think is the most important treatment? You don't have to be a doctor to answer this question. You can just follow the logic. Osteochondrosis is a pathology of the musculoskeletal system. This system is biomechanical in nature. The key word is "mechanical". Consequently, mechanical disorders require the same – mechanical – treatment methods. Therefore, the main type of treatment for osteochondrosis is manual therapy. It is ideally suited for restoring the biomechanics of the musculoskeletal system. And auxiliary methods include medications, physiotherapy, massage, exercise therapy, etc. And it is also important to know that among all types of manual treatment, the safest type is gentle manual therapy. It is superior to conventional manual therapy in its effectiveness, gentleness and safety. To understand what treatment of osteochondrosis by a chiropractor involves, you need to know that intervertebral discs are the only part of the body that does not have blood vessels and is nourished thanks to the proper functioning of the spinal muscles. Failure in the functioning of these muscles immediately impairs the nutrition of the discs. And as we said at the beginning of the article, malnutrition is the very degenerative process of which osteochondrosis is a part.
Effective treatment with gentle manual therapy is fundamentally different from conventional manual therapy. This is not "vertebral realignment" at all, as some people think - it’s something completely different. Gentle manual therapy is a whole system of special methods of influence that eliminate muscle spasms and tension. Return the muscles to their normal physiology and improve the nutrition of the discs.
Observation by a doctor includes three stages:
- Consultation. The doctor finds out what symptoms are troubling the patient, clarifies the medical history, studies the patient’s medical documentation, analyzes images, and determines the nature of the disease.
- Diagnostics. Conducts a thorough examination and clinical examination of the patient: visual and myofascial diagnostics; palpation of tense muscles and painful vertebrae; neurological reflex testing and muscle testing.
- Treatment plan. Based on the history of the current disease, examination data, as well as the results of a clinical examination of the patient, the doctor makes a diagnosis and selects treatment options. The doctor tells the patient in detail about the essence of the disease and the principles of treatment, and answers all the patient’s questions.
Prevention of osteochondrosis
Prevention is necessary to avoid relapses. To do this, you need to create comfortable conditions for work and rest. Maintain physical activity. Avoid overwork. Monitor proper nutrition and weight. But the main thing is not to neglect your health.
Remember, prevention is, first of all, medical supervision and timely correction of the musculoskeletal system. Try to visit a chiropractor at least once every three to six months. This will reduce risk factors and eliminate any violations in a timely manner. Advanced osteochondrosis leads to complications - protrusions and disc herniations. Don't forget this. Take care of yourself!


















